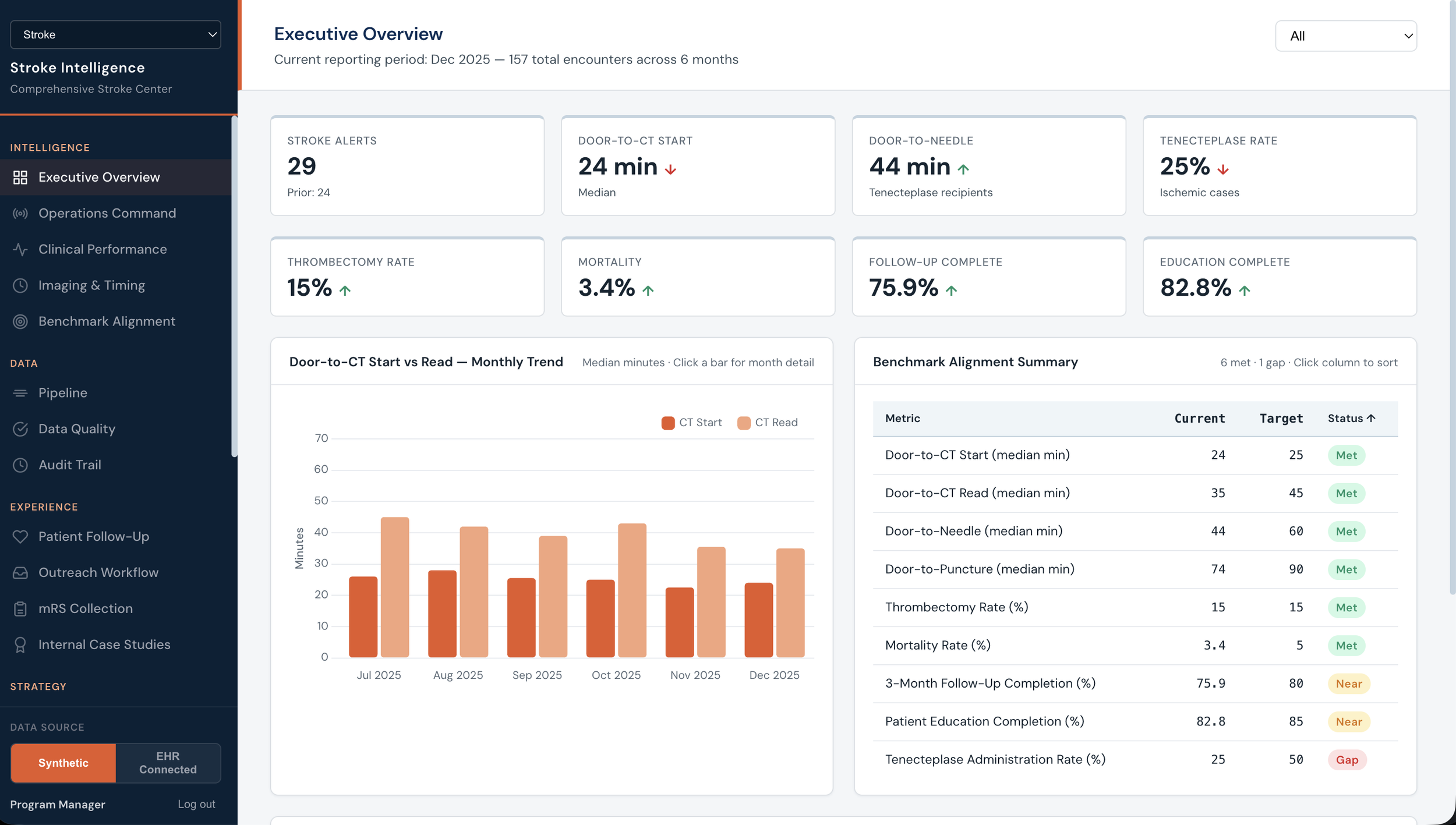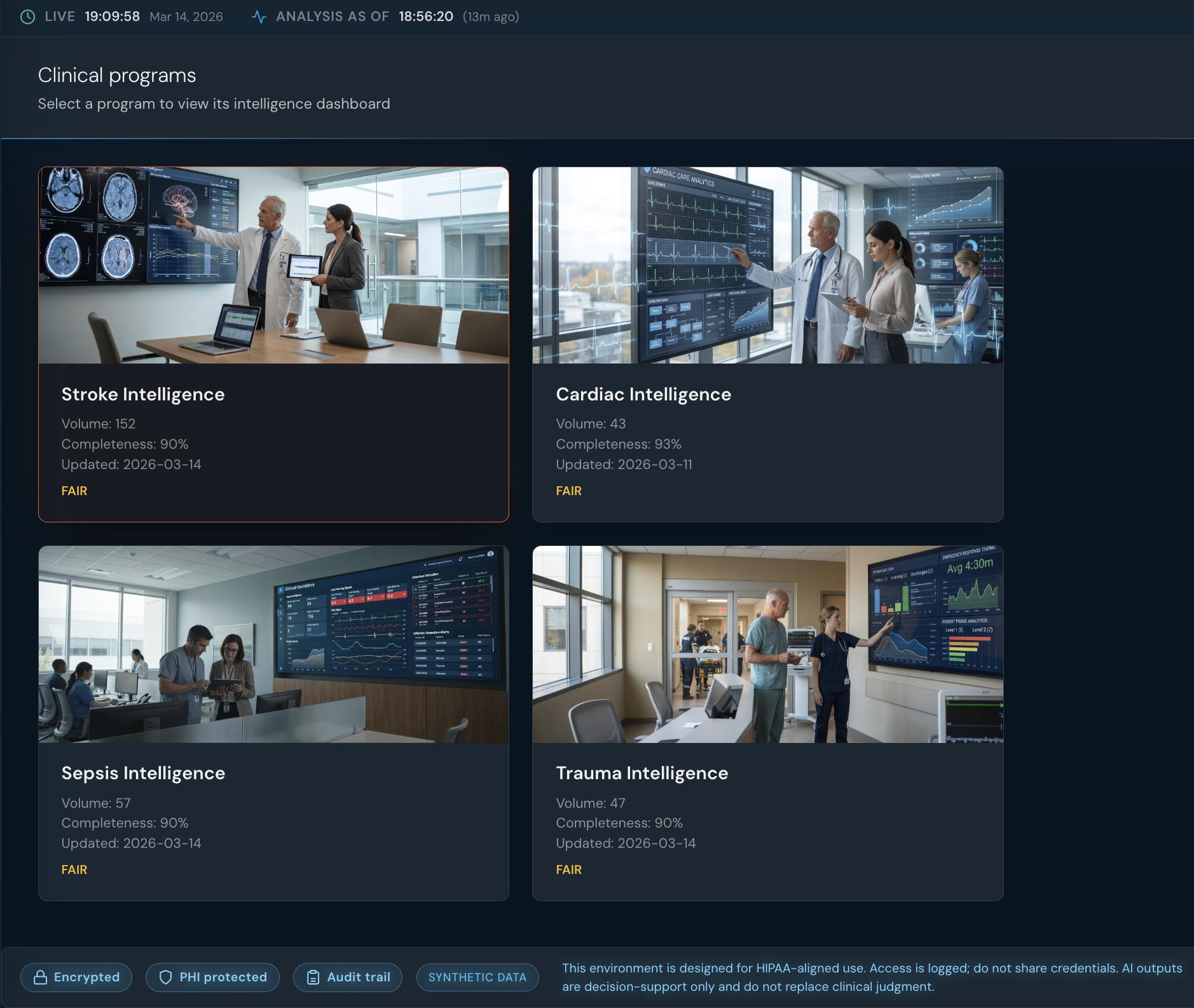
Lumen Stroke Intelligence
Real-time clinical intelligence for the most critical minutes in stroke care.
A CORE FLOW℠ Program Implementation.
Made Possible byVCU Health
HCA Healthcare
AI Ready RVA
Modern Ancients
Every minute of untreated stroke results in the loss of approximately 1.9 million neurons.
Hospitals have the data needed to act quickly.
Lumen helps teams interpret that data when seconds matter most.
Stroke Treatment is a Race Against Time
Stroke care requires rapid coordination between emergency physicians, neurologists, imaging teams, and nurses.
But critical information is often scattered across systems.
• patient history
• imaging results
• lab data
• treatment protocols.
Clinicians must synthesize this information under intense time pressure.
Each stage shows how delays accumulate.
Modern Ancients PresentsThe Lumen System
A bold reimagining of a Stroke Program Managers Intelligence Workflow.
EHR Integration
Displays:
medical history
medications
contraindications.
Explanation:
Critical patient context appears instantly within the stroke evaluation process.
EMS Data
Shows pre-hospital information:
symptom onset
ambulance assessment
transport timing.
Explanation:
Lumen integrates EMS data into the hospital decision timeline.
Lumen Intelligence Engine
This module is the heart of the system.
It explains:
data aggregation
protocol alignment
decision intelligence
workflow monitoring.
Visual:
Animated flow diagram.
Imaging Integration
Shows CT and MRI signals.
Explanation:
Imaging results feed directly into Lumen’s decision synthesis layer.
"Creative, reliable, and genuinely passionate about resolving employee pain-points in healthcare."
Charles Dority | Stroke Program Manager, HCA Healthcare, Chesterfield Virginia
Origin of the Initiative
The AI Ready RVA Healthcare & AI Cohort
The Lumen Stroke Intelligence System concept did not begin in a corporate boardroom or a technology lab. It emerged from a collaborative learning environment designed to explore how artificial intelligence can be applied to real-world healthcare challenges.
The initiative traces its origin to the AI Ready RVA Healthcare & AI Cohort, an educational program bringing together clinicians, researchers, technologists, and community innovators to explore practical applications of AI in healthcare.
Hosted at the Virginia Commonwealth University School of Pharmacy, the cohort created an environment where participants could move beyond theoretical discussions and begin experimenting with real problems.
The session that sparked the Stroke Intelligence concept was a workshop titled:
“Vibe Coding for Healthcare Professionals.”
The event was facilitated by Dayanjan Wijesinghe, Associate Professor in the Department of Pharmacotherapy and Outcomes Science at VCU.
Dr. Wijesinghe’s work spans multiple domains of biomedical research, including lipid signaling in inflammation, drug discovery, precision medicine, and advanced analytical platforms such as LC tandem mass spectrometry. His research program emphasizes the integration of advanced computational tools with biological insight to accelerate scientific discovery.
The workshop itself reflected that philosophy: practical, hands-on exploration of AI systems designed to support real-world scientific and healthcare challenges.
-
The session introduced participants to a different approach to learning and working with AI.
Rather than traditional programming instruction, the workshop emphasized “vibe coding”—a conversational method of building systems with AI as a collaborative partner.
Participants explored concepts including:
AI-assisted reasoning with complex datasets
Notebook-style workflows for exploratory analysis
Practical AI tools such as Claude Code for rapid artifact generation
Scalable frameworks applicable to healthcare and biomedical researchThe session emphasized low-friction learning, enabling professionals to develop intuition for AI systems while engaging directly with their own domains of expertise.
This method recognizes a practical reality: healthcare professionals rarely have the time to pursue extensive technical training while managing demanding clinical responsibilities.
Instead of “finding time” for AI training, the workshop demonstrated how AI could become part of everyday problem-solving.
-
During the session, stroke program subject matter expert Charles joined Alexander Whiteway in a live problem exploration exercise.
Charles did not bring a laptop to the session, so the two participants collaborated directly at a single workstation.
Charles contributed clinical insight into how stroke alerts unfold operationally within hospital environments. Alexander translated those insights into a rapidly evolving system prototype through live coding with AI tools.
This collaborative process surfaced a key realization.
The stroke workflow produces a rich set of operational signals—door-to-CT timing, imaging interpretation, treatment windows, and recovery outcomes—but these signals are typically visible only after cases have concluded through retrospective reporting.
Within minutes of experimentation, the group began exploring what it would look like if those signals could instead be visualized in real time.
That moment marked the beginning of the Stroke Intelligence System concept.
-
The origin of this idea illustrates the power of local innovation ecosystems.
The AI Ready RVA program created a space where multiple sectors could intersect:
Universities
Healthcare institutions
Community initiatives
Startups and technologists
Each group brings a different form of expertise.
Universities contribute research depth and scientific rigor.
Healthcare professionals bring real-world operational insight.
Community programs create spaces where experimentation can occur outside the constraints of traditional institutional processes.
Entrepreneurs and systems designers translate insights into working prototypes.
When these groups interact, ideas that might otherwise take years to emerge can surface in a single collaborative session.
-
Programs such as AI Ready RVA recognize a fundamental shift in how professionals engage with emerging technologies.
The traditional model of technical education—long courses and specialized training—often does not align with the realities of healthcare practice.
Instead, the workshop introduced a method built around three principles:
AI as a Partner
Move beyond traditional coding and treat AI systems as collaborative learning partners.
Low-Friction Learning
Develop intuition and vocabulary through conversational interaction with AI tools.
Expert-Guided Inquiry
Use structured frameworks such as AGIL to stay on productive investigative paths while avoiding technical rabbit holes.
This approach allows professionals to experiment with AI in ways that connect directly to their daily work.
-
The Stroke Intelligence System represents one example of what can emerge from this kind of environment.
A casual collaborative exercise between a clinical expert and a systems designer quickly revealed an opportunity to rethink how stroke care workflows might be visualized and improved.
What began as an experiment in AI-assisted exploration evolved into a broader concept for a real-time operational intelligence platform capable of improving coordination, learning, and patient outcomes within stroke programs.
-
Innovation in healthcare rarely occurs in isolation.
It emerges at the intersection of disciplines, institutions, and communities.
Programs like AI Ready RVA demonstrate how universities, healthcare systems, and community innovators can work together to explore new possibilities.
Rather than “dancing between raindrops” trying to find time for AI education, these environments allow professionals to integrate AI exploration directly into the problems they already care about solving.
The Stroke Intelligence System concept is a direct product of that environment.
And it illustrates how collaborative learning spaces can become catalysts for real-world healthcare innovation.
Why This Idea Emerged in Richmond
Innovation often emerges where diverse institutions intersect and where individuals from different domains have the opportunity to collaborate in unexpected ways. Richmond provides a particularly fertile environment for this kind of interaction. The city is home to major healthcare institutions, research universities, nonprofit organizations, and a growing community of entrepreneurs and technologists. These groups frequently interact through shared educational programs, innovation initiatives, and regional partnerships One of the most influential contributors to this environment is Virginia Commonwealth University, whose schools of medicine, pharmacy, engineering, and health sciences serve as anchors for biomedical research and healthcare innovation. Through programs such as AI Ready RVA, professionals across disciplines have opportunities to explore how artificial intelligence can support real-world challenges in medicine, research, and public health.
These programs bring together participants from different sectors:
University researchers
Healthcare practitioners
Community organizations
Startup founders
Technology professionals
The result is a collaborative ecosystem where ideas can move rapidly from concept to experimentation.
The session that sparked the Lumen Stroke Intelligence System illustrates this dynamic clearly.
A biomedical research scientist facilitating an AI learning workshop,
A stroke program expert sharing operational insight,
And a systems designer translating those insights into a prototype
—all converged in a single room.
This kind of cross-disciplinary interaction is difficult to manufacture through formal institutional processes alone. It often emerges through community-driven initiatives that create space for experimentation and conversation.
In Richmond, the proximity of academic research, clinical practice, and civic innovation has created exactly that kind of space.
The lesson extends beyond a single idea.
Regional ecosystems that connect universities, healthcare institutions, community programs, and entrepreneurial networks can become powerful engines for practical innovation.
When these environments function well, they allow professionals to explore new technologies not as abstract concepts but as tools for solving problems that affect real people in their communities.
The Lumen Stroke Intelligence System began as a simple collaborative experiment during a workshop session.
Yet the idea it represents reflects something much larger: a model for how local ecosystems can contribute to the future of healthcare innovation.
By bringing together clinical expertise, research insight, and emerging AI tools, communities like Richmond can help shape the next generation of intelligent healthcare systems. And sometimes, those transformations begin in the most unexpected ways. With a conversation, a shared laptop, and a willingness to explore what might be possible.
Let’s Work Together
If you're interested in working with us, complete the form with a few details about your project. We'll review your message and get back to you within 48 hours.